
Tele-Speech Remediation of Stuttering: A Case Study
New Case Study : Tele-Speech Remediation of Stuttering
Stuttering affects 1% of the total adult population and is a complex multi-dimensional speech disorder whose impact crosses into an individual’s social, cognitive, emotional, and physiological life (Yairi and Ambrose, 2005). Stuttering or stammering is the disruption in the forward flow of speech. It manifests as repetitions, prolongations, hesitations, blocks, and disruptions in the person’s speech. Further, it is accompanied by secondary behaviors such as eye blinking, body movements, jaw jerks, articulatory fixations, and other physical signs which may or may not be visible to the listener. Negative feelings, depression, and anxiety are commonly associated with stuttering.
Evidence-based behavioral approaches to treat stuttering focus on achieving fluent speech. Some therapeutic approaches used traditionally are the stuttering modification therapy program, the fluency shaping therapy program, Gradual Increase in Length and Complexity of Utterance (GILCU) program among many other treatment programs.
The purpose of the present study was to document and discuss the tele-speech remediation of a person with stuttering via telepractice.
Clinical insights into our client's stuttering remediation journey with us.
Method
Participant
A 25-year-old adult female with a diagnosis of severe stuttering was considered for this study. Written consent was obtained from the participant for the purpose of this study. The participant was a graduate student pursuing engineering. The participant reported stuttering was present since childhood, but she did not seek therapy in the past.
Method
The participant was assessed on Stuttering Severity Instrument (SSI-4) including spontaneous speech and reading samples. The scores were as follows: Frequency: 15, Duration: 10; and Physical concomitance: 8. A diagnosis of severe stuttering was made upon detailed evaluation and testing. Stuttering behavior was noted to be severe across all tasks including speaking, reading, monologue, and conversation. The total stuttered words were counted by the clinician as per standard protocol to arrive at the overall scores for SSI-4.
The stuttering behaviors comprised initial syllable and part-word repetitions, prolongations, blocks, and filled pauses accompanied by a fast rate of speech. In addition to the stuttering behaviors, the participant exhibited jaw jerks, frequent eye blinks, movement of upper extremities, and articulatory fixations during moments of stuttering.
Once the evaluation and testing were completed, the participant was advised to undergo speech therapy for Stuttering. The participant enrolled for Fluency Shaping Therapy (Goldiamond, 1965) twice a week (45 minutes/ session) for a period of nine months from January 2022 to September 2022. Assessment and treatment sessions were conducted via telepractice using the Zoom video-conferencing software. The clinician used a Dell intel core i5 laptop with 300mbps and an in-built camera with an external microphone and speaker. The participant used a Hp laptop with 300mbps internet speed with an in-built camera and microphone.
During the treatment session Fluency Shaping Therapy program was followed.
Strategies such as stretched syllable technique, light articulatory contacts, gentle initiation technique, continuous phonation, and passive airflow technique were incorporated during the treatment sessions. The participant attended once a monthly generalization session (60 minutes) with a group of stuttering individuals on the zoom video-conferencing platform monitored by a clinical psychologist.
A video and audio recording was done during the first assessment session and on the last day of the therapy session to note progress.
The participant’s stuttering was regularly evaluated every three months and the progress was documented.
Results
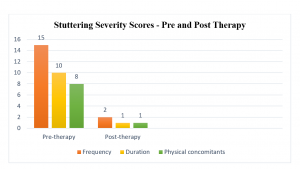
A pre-therapy and post-therapy score assessment was done to determine progress. The stuttering severity instrument (SSI-4) was re-assessed at the end of nine months of intensive stuttering therapy. Graph 1 shows the pre-therapy and post-therapy scores on Stuttering Severity Instrument – 4 (SSI-4).
Graph 1: Pre and Post Therapy scores of frequency, duration, and physical concomitants
Results showed a significant improvement in the overall severity of stuttering in the participant. Post therapy the scores were as follows: Frequency: 2, Duration: 1, and Physical concomitance: 1. The post-therapy score was within the mild stuttering severity on SSI-4. The participant showed positive progress in the overall fluency of speech. Stuttering disruptions such as repetitions, prolongations, blocks, and filled pauses were significantly reduced post-therapy.
Discussion and Conclusion
Stuttering is a speech disorder that affects millions of people around the world. It can cause disruptions in speech fluency, with repetitions, prolongations, or blocks of sounds or words. Stuttering can have a significant impact on a person's social, emotional, and psychological well-being. However, with the right therapy approach, individuals who stutter can learn to manage their stuttering and improve their communication skills.
Stuttering is a long-term multifaceted speech disorder; which manifests itself in surface observable behaviors (i.e., sound repetitions, prolongations, blocks, etc.,) and deeper covert behaviors (i.e., avoidance of speaking, reduced participation, etc.,). The purpose of the current study was to describe tele-speech remediation of an adult with stuttering. The results of the present study indicate positive progress in the overall speech fluency of the participant. The scores of stuttering frequency, duration, and physical concomitants reduced significantly post-therapy conducted via telepractice.
Click here to read more case studies
The Tele-Speech Remediation carried out included strategies from Fluency Shaping Therapy which yielded positive progress. Further, this study revealed telepractice for stuttering remediation resulted in positive progress in the speech fluency of the participant.
- Tele-Speech Remediation of Stuttering: A Case Study - April 22, 2023
- Voice Changes During Puberty in Teenagers - April 11, 2023
- Vital Stim Therapy for Swallowing Difficulty - April 4, 2023

Leave a Comment
(0 Comments)